One of the common clinical scenarios I encounter as a neurosurgeon is a patient who has persistent and severe pain in the back or the legs after a previous surgery on the spine. This is sometimes referred to as “failed back surgery syndrome,” and it occurs in about 20-40% of patients who have had surgery on their spine. The term “failed back surgery syndrome” is somewhat of a misnomer; it’s not meant to imply that there was a problem with a patient’s surgery but rather that the pain has persisted despite surgery.
A number of studies have suggested that for patients with symptoms of failed back syndrome, additional surgeries on the lumbar spine (e.g. laminectomies or fusions) are unlikely to provide satisfactory pain relief.
For patients with features of failed back syndrome, pain relief may be better addressed with a different therapy called spinal cord stimulation. This is a therapy in which we apply targeted pulses of electricity to the spinal cord and nerves to interrupt abnormal pain processing that occurs in the nervous system.
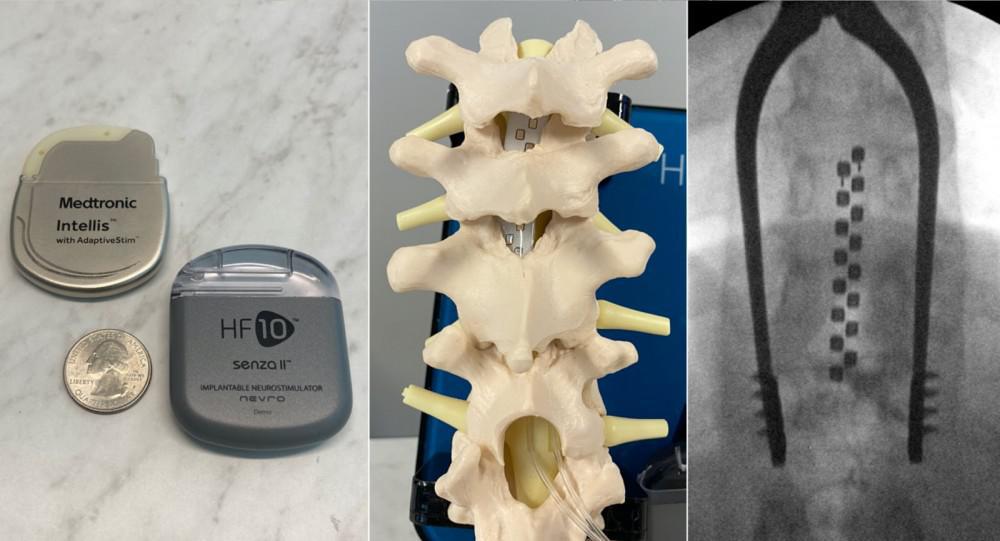
A spinal cord stimulator system consists of two parts. The “business” end of the system consists of one or two wires that enter the spinal canal beneath the bones but above the spinal cord. These wires deliver the electrical impulses to the nervous system. The ends of the wires travel outside of the spine into the soft tissue in the back and are connected to a small battery. Below are example photographs and an X-ray.
Before surgery, I meet with each patient, listen to his or her symptoms, perform a physical examination, and review an MRI scan to understand whether spinal cord stimulation is likely to help. I refer patients to another doctor called a pain psychologist. This doctor meets with you and performs testing to make sure that there aren’t other reasons that you’re having pain that we might treat in a different way. The pain psychology evaluation is an important step in the process, and it is required by insurance companies.
Spinal cord stimulation surgery is performed in two stages:
Stage 1: Trial
This is an outpatient procedure, meaning that you are able to go home on the day of surgery. I use a needle to introduce one or two wires into the spine. The wires exit through the skin and are connected to an external battery pack. You go home with a battery pack and you spend about two weeks determining whether the stimulator reduces your pain. I like for patients to try the stimulator for two weeks because modern systems are very sophisticated, and it is often a process of trial and error to decide which settings provide you the most relief. After two weeks, you return to my office and I pull the wires out. We then have a discussion about how much the stimulator helped you. Patients who have had at least a 50% reduction in their pain have the option of moving forward with a permanent implant (stage 2).
Stage 2: Permanent implant:
The second stage of the surgery is very similar to stage 1, except we implant the entire system (both the wires and the battery) underneath the skin. I often also do this as an outpatient procedure. The battery is rechargeable; you are provided with a device that allows you to charge wirelessly.
Like other forms of neuromodulation that I offer, spinal cord stimulation has been supported by multiple randomized control trials – the gold standard in medicine. Patients who receive spinal cord stimulation report not only improvements in their back and leg pain but also other benefits like reduced opioid use, better functional status, and improved quality of life.
You may be a candidate for spinal cord stimulation if you have persistent and severe pain in your back, neck, arms, or legs after a previous operation on your spine. Spinal cord stimulation can also be used for other disorders like complex regional pain syndrome (CRPS) and peripheral neuropathy. I consider a number of features of your pain and medical history when weighing spinal cord stimulation; we discuss these in more detail at your office visit.